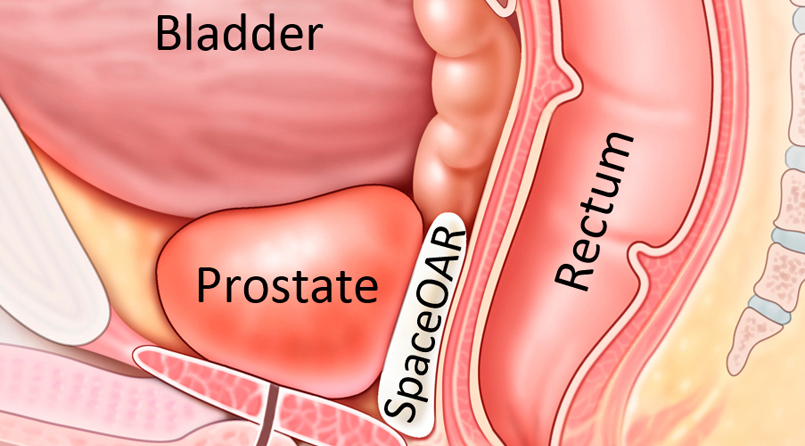
Prostate cancer treatment involves a variety of approaches aimed at managing and potentially curing the cancer while minimizing side effects and preserving quality of life. The choice of treatment depends on factors such as the stage and aggressiveness of the cancer, the patient's overall health, and individual preferences. Some common treatment options for prostate cancer include:
Active Surveillance: For some men with low-risk prostate cancer, especially those with a shorter life expectancy or other health concerns, active surveillance may be recommended. This approach involves closely monitoring the cancer through regular check-ups, prostate-specific antigen (PSA) tests, digital rectal exams (DRE), and periodic biopsies. Treatment may be deferred unless there is evidence of disease progression.
Surgery (Radical Prostatectomy): Radical prostatectomy involves the surgical removal of the entire prostate gland and surrounding tissues. This procedure may be performed using open, laparoscopic, or robotic-assisted techniques. Surgery is most commonly recommended for men with localized prostate cancer who are otherwise healthy and have a life expectancy of more than 10 years. Potential side effects of surgery may include urinary incontinence, erectile dysfunction, and changes in ejaculatory function.
Radiation Therapy: Radiation therapy uses high-energy beams to target and destroy cancer cells in the prostate gland. External beam radiation therapy (EBRT) delivers radiation from outside the body, while brachytherapy involves the placement of radioactive seeds directly into the prostate. Radiation therapy may be used as a primary treatment for localized prostate cancer or as adjuvant therapy after surgery. Side effects of radiation therapy may include urinary problems, bowel changes, and erectile dysfunction.
Hormone Therapy (Androgen Deprivation Therapy): Hormone therapy aims to reduce the levels of male hormones (androgens), such as testosterone, which can fuel the growth of prostate cancer cells. This may involve medications that block the production or action of androgens, surgical removal of the testicles (orchiectomy), or luteinizing hormone-releasing hormone (LHRH) agonists or antagonists. Hormone therapy may be used alone or in combination with other treatments for advanced or metastatic prostate cancer. Side effects of hormone therapy may include hot flashes, fatigue, loss of libido, and osteoporosis.
Chemotherapy: Chemotherapy involves the use of drugs to kill cancer cells or slow their growth. Chemotherapy may be recommended for men with advanced or metastatic prostate cancer that has spread to other parts of the body. Commonly used chemotherapy drugs for prostate cancer include docetaxel, cabazitaxel, and mitoxantrone. Chemotherapy may be used in combination with hormone therapy or other treatments. Side effects of chemotherapy may include nausea, vomiting, hair loss, and increased risk of infection.
Immunotherapy: Immunotherapy is a type of treatment that stimulates the body's immune system to recognize and attack cancer cells. Immunotherapy drugs such as sipuleucel-T (Provenge) may be used for certain men with advanced prostate cancer that has not responded to other treatments. Side effects of immunotherapy may include flu-like symptoms, fatigue, and infusion reactions.
Targeted Therapy: Targeted therapy drugs are designed to target specific molecules or pathways involved in cancer growth and progression. For example, drugs that target the androgen receptor, such as enzalutamide and abiraterone, may be used for men with advanced prostate cancer that has become resistant to hormone therapy. Other targeted therapies may be used in clinical trials or in combination with other treatments. Side effects of targeted therapy may vary depending on the specific drug used.
Clinical Trials: Clinical trials are research studies that evaluate new treatments or treatment combinations for prostate cancer. Participating in a clinical trial may provide access to cutting-edge treatments that are not yet widely available and may help advance scientific knowledge about prostate cancer treatment. It's important to discuss the potential risks and benefits of participating in a clinical trial with a healthcare provider.
The optimal treatment for prostate cancer depends on individual factors such as the stage and aggressiveness of the cancer, the patient's overall health and preferences, and the expertise of the healthcare team. It's essential for men diagnosed with prostate cancer to discuss treatment options with a multidisciplinary team of healthcare providers, including urologists, radiation oncologists, medical oncologists, and other specialists, to develop a personalized treatment plan tailored to their specific needs and circumstances. Early detection and timely intervention are crucial for achieving the best possible outcomes in prostate cancer treatment.